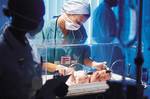
Steroids for mum offer benefits to pre-term babies
 Obstetrics & Gynaecology Obstetrics & Gynaecology
A major international study led by University of Adelaide researchers has confirmed the benefits for premature babies of giving their pregnant mothers repeat doses of corticosteroids. The study, now at the two-year follow-up stage, has shown no harm from repeat doses of corticosteroids given to mothers at ongoing risk of very premature birth (before 32 weeks). At two years of age, the children are showing no adverse effects from the corticosteroids. Study leader Professor Caroline Crowther from the University of Adelaide's Discipline of Obstetrics & Gynaecology says the initial results of the trial showed that repeat doses of corticosteroids reduced breathing and other respiratory problems in the premature babies. There had been concern, however, that such treatments could inhibit the babies' later growth and development. "Our new results show that at two years old the children born to mothers who were given repeat corticosteroids were no more likely to have health or development problems than those born to women who weren't given the repeat doses," said Professor Crowther, who is based at Adelaide's Women's and Children's Hospital. "There were no differences seen between the study treatment groups for body size measurements of weight, height and head circumference. "Our recommendation from these latest results is that given the clear early health benefits shown for babies, without harm at two years, repeat corticosteroids can be considered beneficial where women are still at risk of very pre-term birth a week or more after the first course of corticosteroids." These results have been published in the international journal The New England Journal of Medicine. The study, known as the Australasian Collaborative Trial of Repeat Doses of Steroids, or ACTORDS, is the largest in the world to date, with 982 women and their babies recruited, and involving 23 hospitals in Australia and New Zealand. The two-year follow up assessed 1047 (96%) of the children involved in the trial. The children were seen by a paediatrician and a developmental psychologist, who assessed vision and hearing, developmental milestones, body size, blood pressure, behaviour and general health. "Until now there has been a lack of high-quality evidence, from well-designed, large randomised clinical trials, assessing the efficacy and safety of repeat doses of betamethasone given to women at ongoing risk of very pre-term birth, and no reports on the health of the children later," Professor Crowther said. Earlier results in the study showed that babies born to women who received repeat corticosteroids were less likely to have respiratory problems after birth and breathing problems were less likely to be severe. These babies were also less likely to have other serious health problems than babies whose mothers did not receive repeat corticosteroids. The next step in the study is the early school-age follow up for the children enrolled in the ACTORDS trial, to provide information about the later health and development of the children. This part of the study is now funded by the National Health & Medical Research Council (NHMRC). Within Australia, almost 3% of all births are very pre-term at less than 34 weeks gestation. Babies born early often have respiratory problems and require neonatal intensive care. Not all babies born early survive and those that do are at increased risk of later developmental problems. Researchers are looking for a means of reducing these difficulties. All women recruited to this study had already been given corticosteroids a week or more before. A single course of corticosteroids is known to reduce the risk of respiratory disease and other problems in pre-term babies. The trial was coordinated by a group of researchers from the University of Adelaide's Discipline of Obstetrics and Gynaecology and Discipline of Public Health; Perinatal Medicine at the Women's and Children's Hospital, Adelaide; the Department of Obstetrics and Gynaecology at the University of Melbourne; and the Liggins Institute at the University of Auckland. Funding was obtained from the NHMRC, the Women's and Children's Hospital Research Foundation and the Channel 7 Children's Research Foundation of South Australia. Story by Robyn Mills
|