Simulation Trifecta in Veterinary Education
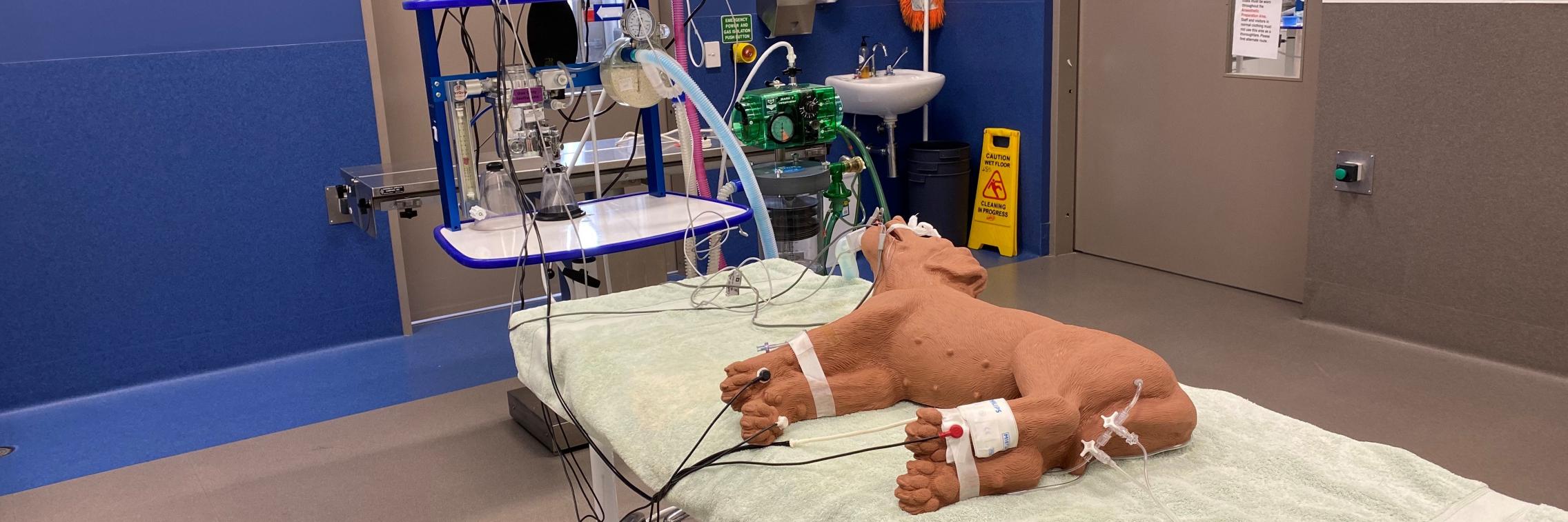
Integrating clinical reasoning, advanced clinical communication and technical skill development.
Clinical veterinary education has traditionally used an apprenticeship model of training in which senior students learn case management and clinical decision-making skills through observation and discussion in the teaching hospital. However, this model is potentially inadequate as it provides little opportunity for skill acquisition due to limited intentional skill practice.
Essentially, observing skills does not yield the same outcomes as practicing skills. In response to some of the limitations for student learning in clinical practice, simulation has become increasingly attractive as an educational alternative in many settings.
- Simulation can be repeated multiple times, allowing the learner to determine the best approach through skills based experience rather than didactic instruction. Patient safety concerns clearly preclude this type of ‘‘trial and error’’ approach to on the floor clinical training.
- It also provides a ‘‘safe zone’’ for the learner in which he or she may experiment with different approaches without fear of making the wrong choice and harming a patient or negatively affecting a client.
- Simulation also reduces animal use and thus helps educators achieve animal welfare imperatives.
- Learners can practice and demonstrate their capacity for effective, efficient and supportive communication with colleagues and clients.
- An integral but often overlooked or deemphasised aspect of simulation is feedback and debrief. Debrief and feedback facilitated by a skilled educator can elevate the simulation from mere technical advancement to an integrated reflection on clinical skill including communication, clinical reasoning, and self-development needs.
Traditional Cardiopulmonary Resuscitation (CPR) Training
Cardiopulmonary resuscitation (CPR) entails medical algorithms, clinical reasoning, technical skills and also the ability to successfully communicate with colleagues in the resuscitation team. However, the classical cornerstone of successful CPR training in veterinary medicine has often excluded the practice, feedback and assessment of communication between team members. Increasing evidence suggests that human factors, including team interaction, communication, and leadership, also influence the performance of CPR (Hunziker et al. 2010). Therefore, there is an educational gap that can be met with simulation to include the medical and technical skills of CPR alongside interprofessional team communication. To capture the complexity of a clinical case, the addition of a simulated client/owner further elevates simulation as a high impact educational tool. The possibilities for integrated simulation in veterinary medicine are endless, exciting and promising.
Clinical Communication Skills in Veterinary Medicine
How often are communication concepts and skills considered, explicitly taught and deliberately integrated into a learner’s assessment or skills activity? And how often do they become the main focus of a simulation activity?
There’s little doubt that clinical communication is an important skill for veterinarians. It is critical for relationships with clients, colleagues and the community. Communication is arguably a core clinical skill yet it is not always taught with the same rigor as other clinical skills. Evidence based teaching methods utilizing simulation with feedback and practice have be only more recently incorporated in veterinary schools in Australia, the UK and North America and with varying levels of adoption. Poor communication has been identified as a contributing cause of medical errors in humans. (Meisel et al. 2015). The consequences of poor communication amongst vets to patient safety has not been investigated in depth. A survey of recent veterinary graduates suggests that 78% of respondents admitted to making errors (Mellanby and Herrtage, 2004). The subjects of the study identified communication breakdowns between colleagues as one the most common causes of their mistakes. In a more recent study, Oxtoby et al. (2015) investigated the most common causes of error from record review of claims made to a profession's indemnity insurer. Again, lack of communication was found to be a leading cause of mistakes. Ineffective communication included poor transfer of information at clinical handovers, a failure to speak up to senior members of staff or to ask for help from colleagues. Thus integrating team communication as a learning outcome in simulation is potentially critical in helping learners increase patient safety as well as team effectiveness.
Breaking bad news to the client: Veterinarians are frequently called upon to break bad news to clients. It is a complex clinical communication skill that requires an understanding of the client’s perspective or views, expressions of authentic empathy, and respectful disclosure of the medical information delivered at just the right time for the client. A particularly challenging communication scenario involves advising a client their animal has died. The client will often experience grief at the loss of their animal and likely the veterinarian will be emotionally affected too. Simulation provides a safe learning environment for learners to practice this set of critical of skills and to help the learner foster an increased perception of competence in managing emotionally charged conversations. Increasing competence in effective communication is likely to have a positive impact on wellbeing as the two are likely inextricably linked.
Simulation as an opportunity for an integrated and holistic educational experience in the Doctor of Veterinary Medicine Program at University of Adelaide
Our primary motivation for developing an integrated simulation practical was to provide an opportunity for final year veterinary students (DVM3) to practice effective clinical communication with colleagues and clients while also juggling clinical and medical skill application. CPR simulation is a perfect clinical model to address the following:
- It helps assess team dynamics via techniques such as closed-loop communication, knowledge sharing, sensitively communicating safety concerns and interdisciplinary/professional respect.
- It provides an additional opportunity for learners to practice their client communication:
- breaking bad news;
- grief and loss;
- discussion of costs associated with service;
- disclosing error and
- communicating bad news over the phone.
At the end of the simulation session, a debriefing session allows students to critically reflect on their performance in detail and provide opportunities to discuss and process with one another what they have learned. Debriefing sessions also facilitate use of therapeutic communication skills, address students' emotions, and affirm feelings as an integral component of the teaching–learning process (Horsfall, 1990). The debrief helps link learning objectives to the educational experience. Through the debrief process and utilising the data drawn from the simulation, it helps learners make sense of their experience through self-reflection whereby they consider:
- ethical and legal responsibilities
- their learning objectives
- theoretical and empirical data to support their learning
- their emotional reaction to challenging events and conversations,
- moral conflicts
- strategies for self-care in the moment and when they graduate
- and reflect on their medical and technical skill development.
Integrated clinical simulation enhances performance, knowledge, team dynamics and client communication. Overall, creatively incorporating client and team communication to a challenging clinical simulation allowed us to create a more realistic case for the students to navigate. It also provided a mechanism through which we could model effective and growth producing debriefing; an important skill for supporting wellbeing in the workplace.
CPR Team Dynamics


The CPR practical involved a real-time simulation of an emergency arrest incident which promoted critical thinking, clear communication, team work and initiative. It helped us as students practice use of correct protocols in a supportive learning environment, where we gained insight into areas we could improve through provision of constructive feedback.Amber Jurek Class of 2020
Client Communication

Clinical communication is an important skill for veterinarians; simulation provides a safe learning environment for learners to practice this set of critical of skills.
Debriefing

Video-assisted debriefing allows learners to review performance without time-pressure or relying on recollection of events.
By Dr Luiz Santos B.V.Sc, M.Sc., Dip.ACVAA Lecturer – Veterinary Anaesthesiology and Dr Michelle McArthur B.A. (Psych), Hons, D.Clin.Psych. Associate Professor- Veterinary Communication and Wellbeing both from the School of Animal and Veterinary Science.
References
Blackwell MJ. The 2001 Inverson Bell Symposium keynote address: beyond philosophical differences: the future training of veterinarians. J Vet Med Educ 2001; 28:148–152.
Brown JP, Silverman JD. The current and future market for veterinarians and veterinary medical services in the United States. J Am Vet Med Assoc 1999; 215:161–183.
Fletcher DJ, Militello R, Schoeffler GL, et al. Development and evaluation of a high-fidelity canine patient simulator for veterinary clinical training. J Vet Med Educ 2012; 39:7–12
Horsfall J. Clinical placement: Pre-debriefing and debriefing as teaching strategies. Australian Journal of Advanced Nursing 1990; 8 (1):3-7
Hunziker S, Tschan F, Semmer NK, Howell MD, Marsch S. Human factors in resuscitation: Lessons learned from simulator studies. J Emerg Trauma Shock 2010; 3(4):389-394.
Mellanby, R. & Herrtage, M. Survey of mistakes made by recent veterinary graduates. Veterinary Record 2004; 155: 761–765.
Meisel ZF, Smith RJ. Talking back: A review of handoffs in pediatric emergency care. Clinical Pediatric Emergency Medicine 2015;16(2):76-82.
Oxtoby, C., Ferguson, E., White, K., Mossop, L. We need to talk about error: causes and types of error in veterinary practice. Veterinary Record 2015; 177: 438.
